Search
Guideline 11.9 - Managing Acute Dysrhythmias
Introduction

(To be read in conjunction with Guideline 11.7 Post-Resuscitation Therapy in Adult Advanced Life Support)
The term cardiac arrhythmia refers to an abnormality of the heart rhythm. The normal heart rate is usually between 60 and 100 beats per minute. The heart may beat excessively fast (tachycardia or tachyarrhythmia), excessively slow (bradycardia or bradyarrhythmia), and may be in a regular or an irregular pattern (commonly atrial fibrillation).
Both fast and slow abnormalities of the heart rhythm may lead to cardiac arrest. Most (about 80%) cardiac arrests are related to excessively fast rhythms that originate in the lower chambers of the heart (ventricular tachycardia and fibrillation). Complete cessation of all heart electrical activity (asystole) may be seen following a prolonged period of tachycardia or as a result of bradycardia.
Fast rhythms of the heart may respond to synchronized electrical therapy (cardioversion) to reset the normal activity of the heart. They may also respond to drug therapy. Unsynchronised electrical therapy (defibrillation) is the mainstay of treatment of fast rhythms of the heart when the patient is in cardiac arrest.
Slow rhythms of the heart may be treated with drugs to increase the heart rate such as atropine (anti-cholinergic) or adrenergic agents. Alternately, an electrical impulse may be applied to the heart either internally (internal pacemaker) by cardiac pacing wires or externally (external pacemaker) by pads.
All anti-arrhythmic treatments (physical maneuvers, drugs, cardioversion, pacing) have the potential to make the rhythm worse rather than better, causing clinical deterioration. Furthermore most anti-arrhythmic drugs cause myocardial depression, which may worsen heart failure or hypotension.
It is important to recognise patients who are stable and have no adverse signs from an arrhythmia. If there is no immediate urgency for treatment, and especially if there is any uncertainty about the best choice of treatment, seek expert help (eg. cardiology).
Whilst assessing the patient:
- give oxygen and obtain IV access if not already done (particularly if adverse signs are present); and
- record a 12-lead ECG if not already done (without delaying treatment).
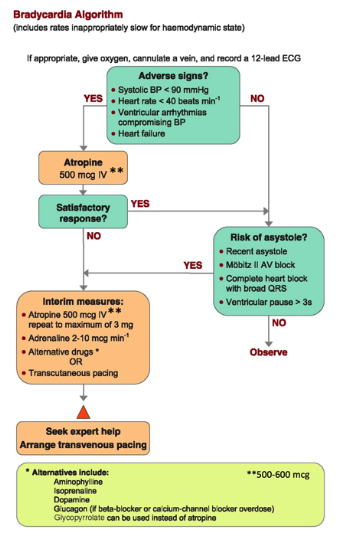
Bradyarrhythmia

The conventional definition of bradyarrhythmia is a heart rate < 60/min; however, for some people or some situations heart rates of < 60/min are not harmful and may be entirely physiological. Patients with a slow heart beat who do not experience symptoms usually do not require emergency therapy. The common symptoms of bradycardia include syncope (fainting), shortness of breath, dizziness or chest pain. The following adverse signs suggest a need for immediate treatment (see bradycardia algorithm):
- systolic BP < 90 mmHg;
- heart rate < 40/min;
- ventricular arrhythmia;
- heart failure.
A pulseless patient with a bradyarrhythmia requires cardiac arrest management according to the cardiac arrest algorithm (see ANZCOR Guideline 11.2).
Drug therapy
Atropine is the initial treatment and is administered intravenously in doses of 500-600 mcg (repeated as necessary every 3-5 min up to a total dose of 3 mg). ( Level of evidence III-2) If this fails low dose adrenaline is the second line agent (as a bolus or as an infusion). Adrenaline is usually administered at a rate of 2-10 mcg/min to maintain a satisfactory heart rate (stable heart rate with a mean arterial pressure of 70 mm Hg). Other drugs that can be given for the treatment of bradycardia include isoprenaline (2-5 mcg/minute), dopamine (2-5mcg/kg/minute, theophylline (Level III-2) and glycopyrrolate. In the presence of therapy with beta blockers much higher doses may be required to overcome the effects of these agents. Consider giving intravenous glucagon [1] or insulin/glucose/potassium therapy [2] if a beta-blocker or calcium channel blocker is the cause of the bradycardia (Level of evidence IV). Do not give atropine to patients with cardiac transplant as the heart is denervated and will not respond to vagal blockade, and there is some risk of inducing paradoxical atrio-ventricular block. [1]
Pacing
Patients who fail to respond to pharmacotherapy, or who are at high risk of asystole, may require electrical pacing (via either an internal or external route). The potential risk of asystole is indicated by the presence of any of the following:
- recent asystole;
- Mobitz II atrioventricular (AV) block;
- complete AV block (3rd degree heart block) (especially with broad QRS or initial heart rate < 40/min);
- ventricular standstill of > 3 sec.
Many defibrillators now have the capacity to provide external pacing via the defibrillation paddles or adhesive pads. External pacing stimulates skeletal muscle as well as cardiac muscle and may produce discomfort to the patient.
The pacing is usually set to demand (as required) at 70-80 beats per minute starting low (eg. 30 mA) and increasing until electrical capture with established output occurs. In some settings (such as pre-hospital) where there is a concern that electrical artifact may inhibit pacing in the demand mode, it is reasonable to use a fixed (asynchronous) mode.
Class of Recommendation A
Reference [1, 3]
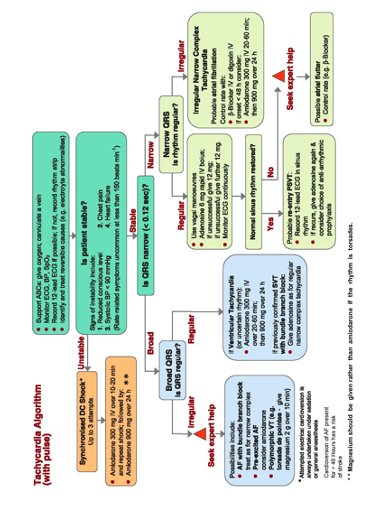
Tachyarrhythmia

A tachyarrythmia may arise from the upper chambers of the heart (atria) or the lower chambers of the heart (ventricular). In the setting of cardiac arrest most arrhythmias will be ventricular in origin. Patients who do not experience symptoms associated with a tachycardia / tachyarrhythmia do not usually require emergency therapy specifically directed at the heart rhythm.
Most sudden cardiac arrests (approximately 80%) occur as a result of abnormally fast and often disorganised electrical activity arising from the ventricle. These arrhythmias are called ventricular tachycardia (VT) when the rhythm is organised and ventricular fibrillation (VF) when the ECG appears to exhibit disorganised electrical activity (due to multiple complex re-entry electrical circuits).
The common symptoms of tachycardia include syncope (fainting), shortness of breath, dizziness, chest pain or palpitations. The following adverse features suggest a need for immediate treatment (see tachycardia algorithm):
- systolic BP < 90 mmHg;
- heart rate > 150/min;
- chest pain;
- heart failure; or
- drowsiness or confusion
A pulseless patient with a tachyarrhythmia requires cardiac arrest management according to the cardiac arrest algorithm (see ANZCOR Guideline 11.2).
In the peri-arrest setting, if the patient is unstable and deteriorating with adverse features caused by the tachyarrythmia, attempt immediate synchronised cardioversion, with sedation as required. If cardioversion is unsuccessful give amiodarone 300 mg intravenously over 10-20 min, then repeat attempted cardioversion. Follow the initial dose with an amiodarone infusion 900 mg over 24 h.
If there are no adverse features during a tachyarrhythmia, determine whether the arrhythmia has narrow (i.e., normal duration) QRS complexes or whether they are broad (0.12 sec or longer). This distinguishes broad-complex tachycardia from narrow-complex tachycardia.
Broad-complex tachycardia
Although broad-complex tachycardia can be a supraventricular tachycardia with aberrant conduction (i.e., bundle branch block), in the peri-arrest setting assume that broad-complex tachycardias are ventricular in origin. Treating a supraventricular tachycardia (SVT) as if it were ventricular tachycardia (VT) is less likely to lead to deterioration than treating VT as SVT.
Regular broad-complex tachycardia
In the absence of adverse features, give amiodarone 300 mg intravenously over 20-60 min, followed by an infusion of 900 mg over 24 h. Continue to monitor and assess the patient, seek expert help, and be prepared to use electrical cardioversion if adverse signs develop, or if the arrhythmia persists for several hours.
Irregular broad complex tachycardia
This is most likely to be atrial fibrillation (AF) with bundle branch block, but careful examination of a 12-lead ECG (if necessary by an expert) may enable confident identification of the rhythm. Other possible causes are AF with ventricular pre-excitation (in patients with Wolff-Parkinson-White (WPW) Syndrome), and polymorphic VT (e.g., “torsades de pointes”). Seek expert help with the assessment and treatment of irregular broad-complex tachyarrhythmia.
If pre-excited AF (or atrial flutter) is suspected, avoid adenosine, digoxin, verapamil and diltiazem. These drugs block the AV node and cause a relative increase in pre-excitation. Electrical cardioversion is usually the safest treatment option.
“Torsades de pointes” is a specific type of ventricular tachyarrhythmia that occurs in the setting of acquired or congenital prolongation of the QT interval on the ECG (repolarisation phase). Torsades may be self limiting or sustained leading to cardiac arrest. Torsades leading to cardiac arrest is managed according to the cardiac arrest algorithm (see ARC Guideline 11.2). Treat torsades de pointes VT immediately by stopping all drugs known to prolong the QT interval and correct electrolyte abnormalities (especially hypokalaemia) and other causes (eg. ischaemia). Give a bolus of 5mmol of magnesium intravenously over 10 min, which may be repeated once and followed by an infusion of 20mmol over four hours.
Acute pacing is recommended for patients presenting with torsades de pointes due to heart block and symptomatic bradycardia. Obtain expert help as other treatment (e.g. including overdrive pacing or isoprenaline) may be indicated to prevent relapse once the arrhythmia has been corrected. If adverse signs develop, arrange immediate synchronised cardioversion. Amiodarone should be avoided as this can make the situation worse.
Summary Recommendations
Sustained Monomorphic Ventricular Tachycardia
Summary Recommendations
Class A
- Wide-QRS tachycardia should be presumed to be VT if the diagnosis is unclear. (Level of Evidence: C)
- Direct current cardioversion with appropriate sedation is recommended at any point in the treatment cascade in patients with suspected sustained monomorphic VT with hemodynamic compromise. (Level of Evidence: IV)
Class B
- Intravenous amiodarone is reasonable in patients with sustained monomorphic VT that is haemodynamically unstable, refractory to conversion with countershock, or recurrent despite other agents. (Level of Evidence: IV)
- Transvenous catheter pacing termination can be useful to treat patients with sustained monomorphic VT that is refractory to cardioversion or is frequently recurrent despite anti-arrhythmic medication. (Level of Evidence: IV)
- Intravenous lignocaine is reasonable for the initial treatment of patients with stable sustained monomorphic VT specifically associated with acute myocardial ischemia or infarction. (Level of Evidence: IV)
- Calcium channel blockers such as verapamil and diltiazem should not be used in patients to terminate wide-QRS-complex tachycardia of unknown origin, especially in patients with a history of myocardial dysfunction. (Level of Evidence: IV)
Torsades de Pointes
Summary Recommendations
Class A
- Withdrawal of any offending drugs and correction of electrolyte abnormalities are recommended in patients presenting with torsades de pointes. (Level of Evidence:III-2)
- Acute pacing is recommended for patients presenting with torsades de pointes due to heart block and symptomatic bradycardia. (Level of Evidence: III-2)
Class B
- Management with intravenous magnesium sulfate is reasonable for patients who present with Long QT Syndrome (LQTS) and episodes of torsades de pointes. Magnesium is not likely to be effective in patients with a normal QT interval. (Level of Evidence:
- Acute pacing is reasonable for patients who present with recurrent pause-dependent torsades de pointes. (Level of Evidence: II)
- Beta blockade combined with pacing is reasonable acute therapy for patients who present with torsades de pointes and sinus bradycardia. (Level of Evidence:IV))
- Isoprenaline is reasonable as temporary treatment in acute patients who present with recurrent pause dependent torsades de pointes who do not have congenital LQTS. (Level of Evidence:II)
Reference [4]
Narrow-complex tachycardia
Narrow-complex tachycardias can be subdivided into regular and irregular types.
Regular narrow-complex tachycardia
Regular narrow-complex tachycardia include:
- sinus tachycardia;
- AV nodal re-entry tachycardia – AVNRT (the commonest type of SVT);
- AV re-entry tachycardia - AVRT (caused by WPW Syndrome); and
- atrial flutter with regular AV conduction (usually 2:1).
If the patient is unstable with adverse signs caused by the arrhythmia (other than sinus tachycardia), attempt synchronised electrical cardioversion, with sedation as required.
It is reasonable to give adenosine to an unstable patient with a regular narrow-complex tachycardia, while preparations are made for synchronised cardioversion. However, do not delay electrical cardioversion if the adenosine fails to restore sinus rhythm.
In the absence of adverse features, start with vagal manoeuvres ( eg. the Valsalva manoeuvre [5]) If the arrhythmia persists and is not atrial flutter, use adenosine. Give 6 mg as a rapid intravenous bolus followed a minimum 20 ml flush. If the ventricular rate slows transiently, but the arrhythmia then persists, look for atrial activity such as atrial flutter or other atrial tachycardia and treat accordingly. If there is no response to adenosine 6 mg give a 12 mg bolus (which may be repeated). If adenosine is contra-indicated or fails to terminate a regular narrow-complex tachycardia without demonstrating that it is atrial flutter, give a calcium channel blocker (e.g. verapamil 2.5-5 mg IV over 2 min; or diltiazem 15-20 mg over 2 min).
Level of Evidence
(Verapamil IV, Diltiazem and beta blockers IV)
Class of Recommendation
Class A
Reference: [6]
Irregular narrow-complex tachycardia
Irregular narrow-complex tachycardia is most commonly atrial fibrillation (AF) or sometimes atrial flutter with variable AV conduction (variable block). Atrial fibrillation is the most common of all arrhythmias arising from the upper chambers of the heart. The arrhythmia is caused by multiple re-entry circuits within the upper chamber usually triggered by ectopic (abnormal) foci located in tissue within the pulmonary veins that empty into the atria. The arrhythmia may arise in an otherwise normal heart or in the setting of major structural abnormalities (especially of the heart valves) or systemic disease states. This arrhythmia occurs with increasing frequency in older patient groups where it is often associated with underlying disease process. The hallmark of this rhythm disturbance is that it produces an irregularly irregular heart rhythm. Atrial flutter is a related but distinct arrhythmia caused by re-entry within the atria. It may be managed similarly to atrial fibrillation in the emergency setting.
If the patient is unstable with adverse signs caused by the arrhythmia, attempt synchronised electrical cardioversion, with sedation as required.
If there are no adverse features, treatment options include:
- rate control by drug therapy;
- rhythm control using drugs to encourage chemical cardioversion;
- rhythm control by electrical cardioversion; and
- treatment to prevent complications (e.g., anticoagulation).
The longer a patient remains in AF the greater the likelihood of atrial clot developing. In general, patients who have been in AF for more than 48 hours should not be treated by cardioversion (electrical or chemical) until they have been fully anticoagulated or unless absence of atrial clot has been shown by trans-oesophageal echocardiography. Obtain expert help to determine the most appropriate treatment for the individual patient.
In the acute care setting the simplest approach to managing this condition is to control the rate of ventricular response. This can be achieved with agents such as oral or intravenous beta blockers (metoprolol 5mg IV) (contraindications would include a history of bronchospasm or evidence of decompensated heart failure) or digoxin (250 mcg to 500mcg IV or PO). In cases of paroxysmal (intermittent) atrial fibrillation many patients revert to a normal heart rhythm spontaneously.
Pharmacological Rate Control During Atrial Fibrillation
Recommendations

Class A
- Measurement of the heart rate at rest and control of the rate using pharmacological agents (either a beta blocker or nondihydropyridine calcium channel antagonist (verapamil, diltiazem) in most cases) are recommended for patients with persistent or permanent AF.(Level of Evidence: II)
- In the absence of pre-excitation, intravenous administration of beta blockers
or nondihydropyridine calcium channel antagonists (verapamil, diltiazem) is recommended to slow the ventricular response to AF in the acute setting, exercising caution in patients with hypotension or HF. (Level of Evidence: II
- Intravenous administration of digoxin or amiodarone is recommended to control the heart rate in patients with AF and HF who do not have an accessory pathway. (Level of Evidence: II)
In patients who experience symptoms related to AF during activity, the adequacy of heart rate control should be assessed during exercise, adjusting pharmacological treatment as necessary to keep the rate in the physiological range. (Level of Evidence: IV)
- Digoxin is effective following oral administration to control the heart rate at rest in patients with AF and is indicated for patients with HF, LV dysfunction, or for sedentary individuals. (Level of Evidence:IV)
Class B
- A combination of digoxin and either a beta blocker or nondihydropyridine calcium channel antagonist is reasonable to control the heart rate both at rest and during exercise in patients with AF. The choice of medication should be individualised and the dose modulated to avoid bradycardia. (Level of Evidence:II)
- Amiodarone can be useful to control the heart rate in patients with AF when other measures are unsuccessful or contraindicated. (Level of Evidence: II)
Class C
- When the ventricular rate cannot be adequately controlled both at rest and during exercise in patients with AF using a beta blocker, nondihydropyridine calcium channel antagonist or digoxin, alone or in combination, oral amiodarone may be administered to control the heart rate. (Level of Evidence: III-2)
- Amiodarone may be considered for hemodynamically stable patients with AF involving conduction over an accessory pathway. (Level of Evidence: III-2)
Class C
- Digoxin should not be used as the sole agent to control the rate of ventricular response in patients with paroxysmal AF. (Level of Evidence: II)
- Intravenous administration of digoxin or nondihydropyridine calcium channel antagonists to patients with AF and a preexcitation syndrome may paradoxically accelerate the ventricular response and is not recommended. (Level of Evidence: IV)
Reference: [7]
References

- 2005 International Consensus on Cardiopulmonary Resuscitation and Emergency Cardiovascular Care Science with Treatment Recommendations. Part 4: Advanced Life Support. Resuscitation. 2005 Nov-Dec; 67(2-3):213-47.
- Shepherd G. Treatment of poisoning caused by beta-adrenergic and calcium-channel blockers. Am J Health Syst Pharm. 2006;63(19):1828-35.
- Advanced Life Support 5th Edition (Australian Edition). Melbourne. Australian Resuscitation Council. 2006
- Zipes DP, et al; American College of Cardiology/American Heart Association Task Force; European Society of Cardiology Committee for Practice Guidelines; European Heart Rhythm Association; Heart Rhythm Society. ACC/AHA/ESC 2006 Guidelines for Management of Patients With Ventricular Arrhythmias and the Prevention of Sudden Cardiac Death: a report of the American College of Cardiology/American Heart Association Task Force and the European Society of Cardiology Committee for Practice Guidelines (writing committee to develop Guidelines for Management of Patients With Ventricular Arrhythmias and the Prevention of Sudden Cardiac Death): developed in collaboration with the European Heart Rhythm Association and the Heart Rhythm Society. Circulation. 2006 Sep 5;114(10):e385-484.
- Wong LF, Taylor DM, Bailey M. Vagal Response Varies With Valsalva Maneuver Technique: A Repeated-Measures Clinical Trial in Healthy Subjects. Ann Emerg Med. 2004;43:477-482.
- Blomström-Lundqvist C, et al; European Society of Cardiology Committee, NASPE-Heart Rhythm Society. ACC/AHA/ESC guidelines for the management of patients with supraventricular arrhythmias--executive summary. A report of the American College of Cardiology/American heart association task force on practice guidelines and the European Society of Cardiology Committee for practice guidelines (writing committee to develop guidelines for the management of patients with supraventricular arrhythmias) developed in collaboration with NASPE-Heart Rhythm Society. J Am Coll Cardiol. 2003 Oct 15;42(8):1493-531.
- Fuster V, et al; American College of Cardiology/American Heart Association Task Force on Practice Guidelines; European Society of Cardiology Committee for Practice Guidelines; European Heart Rhythm Association; Heart Rhythm Society. ACC/AHA/ESC 2006 Guidelines for the Management of Patients with Atrial Fibrillation: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines and the European Society of Cardiology Committee for Practice Guidelines (Writing Committee to Revise the 2001 Guidelines for the Management of Patients With Atrial Fibrillation): developed in collaboration with the European Heart Rhythm Association and the Heart Rhythm Society. Circulation. 2006 Aug 15;114(7):e257-354. Erratum in: Circulation. 2007 Aug 7;116(6):e138.
Further Reading

ANZCOR Guideline 7 Cardiopulmonary Resuscitation
ANZCOR Guideline 11.2 Protocols for Adult Advanced Life Support
ANZCOR Guideline 11.8 Targeted Temperature Management (TTM) after Cardiac Arrest
ANZCOR Guideline 11.7 Post-resuscitation therapy in Adult Advanced Life Support
Bradycardia and Tachycardia Algorithm
Referencing this guideline

When citing the ANZCOR Guidelines we recommend:
ANZCOR, 2025, Guideline 11.9 - Managing Acute Dysrhythmias, accessed 9 July 2025, https://www.anzcor.org/home/adult-advanced-life-support/guideline-11-9-managing-acute-dysrhythmias



